Full Term Feelings: Edward & Harry
Both Edward and Harry were born at full-term with Edward receiving treatment for sepsis and Harry requiring breathing support


Both Edward and Harry were born at full-term with Edward receiving treatment for sepsis and Harry requiring breathing support


Every year, Bliss Charity runs a Full Term Awareness Month campaign to raise awareness of the journeys that families go through when a baby becomes unwell after being born at full-term.
As part of this, families are invited to share their stories using the hashtag #FullTermFeelings. Below, you can read the Greenway family’s story, kindly written by mum, Charlotte. Both Edward and Harry were born at full-term, but went on to spend time in Guernsey’s NICU, now known as the Special Care Unit.
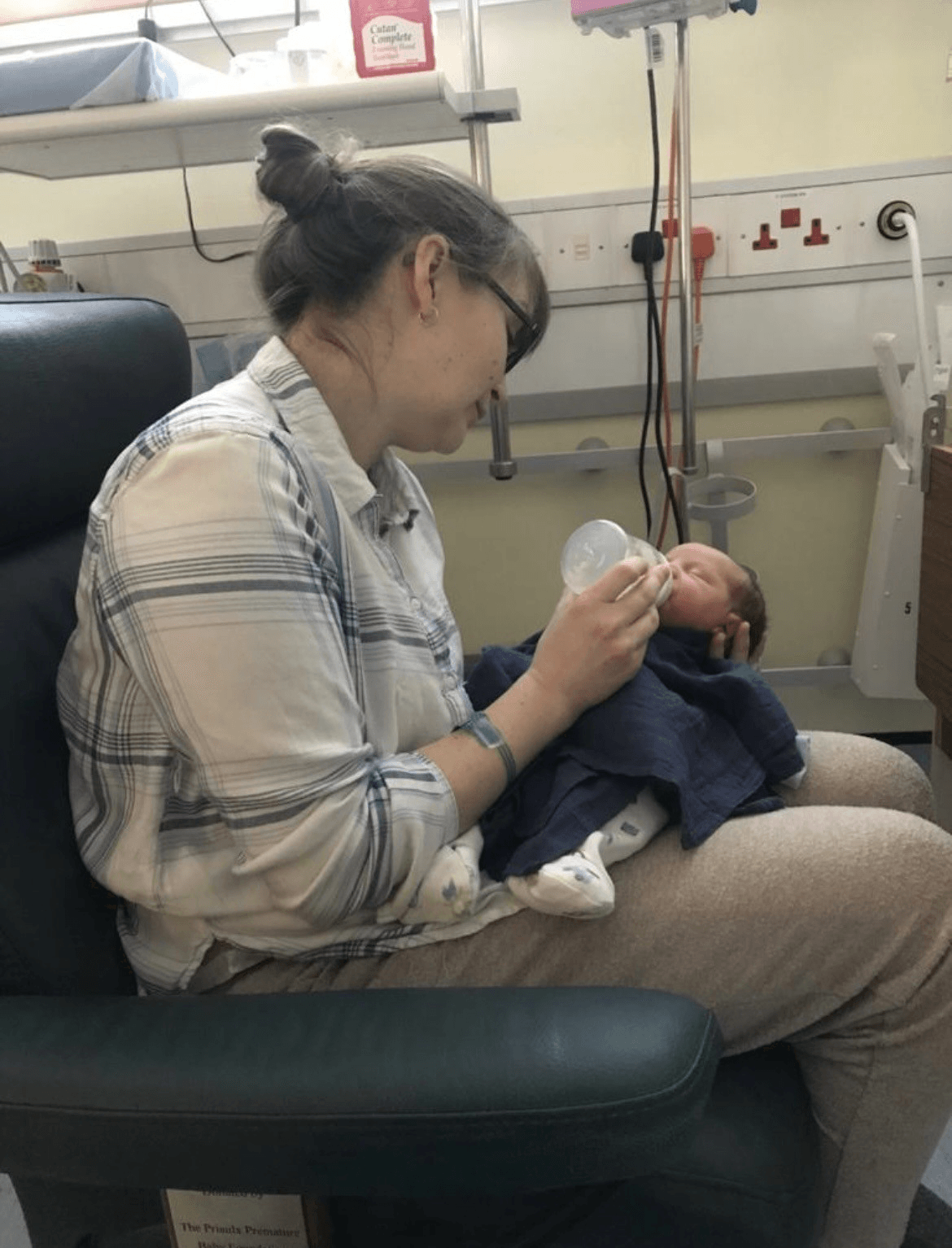
Our son Edward was born at 38 weeks, 4 days. I was induced due to reduced movements but he took 26 hours to arrive – the labour was intense. The day after Edward was born, I happened to mention to the midwife that he was a ‘good baby’ who very rarely cried. This must have rung alarm bells for her. He went for his routine checks and the paediatrician returned to my room without him.
She explained that Edward was very poorly and had been moved into the NICU. His infection markers were 60 when they should be below 10. He spent 18 hours in the ICU (Intensive Care Unit) and the following three days in the room with me, but was taken out every 4 hours for his antibiotics. He was given antibiotics for five days in total for Group B strep sepsis.
According to the Centers for Disease Control, Group B Streptococcus (GBS) is the leading cause of meningitis and sepsis in a newborn’s first week of life. When infection occurs, babies can become dangerously ill and need immediate treatment. With fast and appropriate medical care, many babies do go on to recover fully.

Our son Harry was born naturally at 40 weeks, 5 days. Labour was only 8 hours, and everything seemed fine. Harry was placed in a ‘hot cot’ soon after he was born and he was in there for roughly 12 hours. We were then discharged and went home feeling ecstatic. On our second morning home, my husband Ben and I realised Harry hadn’t woken for a feed in 8 hours and he was spiking a temperature. We rushed him into A&E and he was immediately given a cannula with intravenous antibiotics.
A hot cot (also known as a heated mattress or conductive heating cot) is a specialised medical cot designed to provide an optimal thermal environment for newborns who are struggling to regulate their own body temperature.
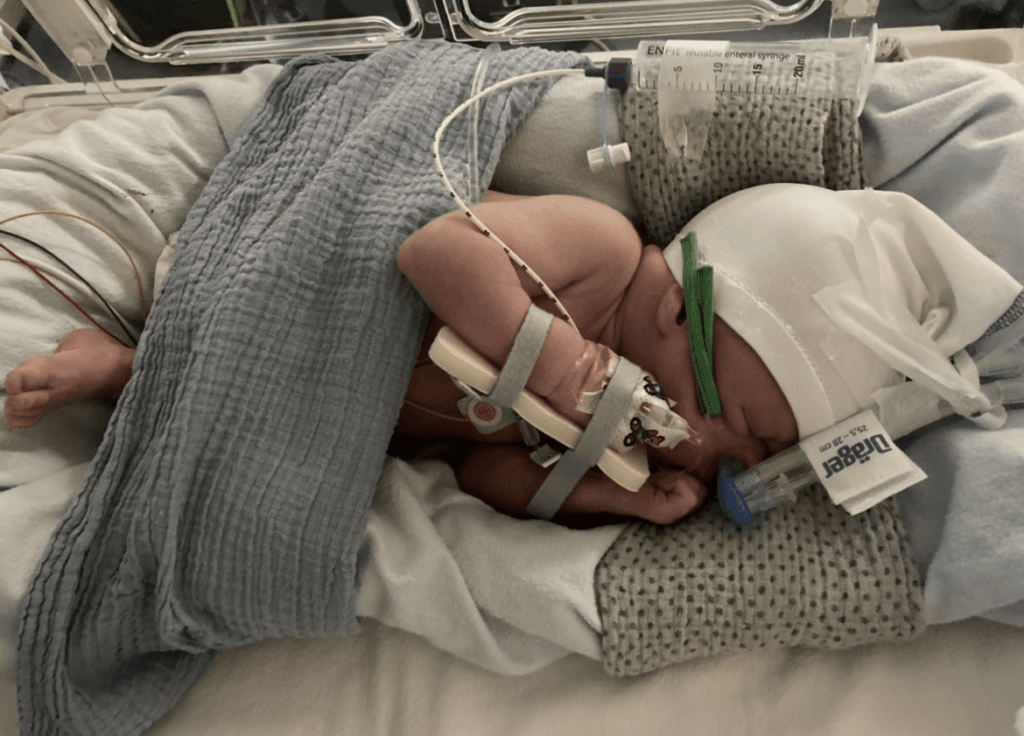
His infection markers were 59 and he had a lumbar puncture done on admission. It was suspected that Harry had sepsis but he stayed with me initially on the ward and he was being monitored frequently. The following day, Harry’s oxygen levels dropped into the 50s and he became blue. The nurses rushed in with alarms going whilst Ben and I were escorted to the family room.
After an hour of waiting, which seemed like an eternity, we were asked to follow the midwife into the NICU and our hearts sank. Harry was on a CPAP* machine which was breathing for him and we were only allowed to place our arm into the incubator.
CPAP stands for Continuous Positive Airway Pressure and is a special type of breathing circuit that is used to help a baby’s breathing.

We were told that if Harry’s oxygen levels keep dropping that he would be flown to Southampton. He was being fed via a nasogastric tube. Harry was then moved to optiflow* for several days and was attempting to bottle feed. Overall Harry was under the NICU care for a week.
Optiflow is a non-invasive, nasal high-flow oxygen therapy system used for infants in respiratory distress, providing warmed, humidified, and blended air/oxygen.

Before we went through these experiences, I had assumed that NICU was simply for premature babies. As traumatic as both these experiences were, Ben and I cannot thank the incredible Staff who saved our Boys’ lives – we are, and always will be, eternally grateful!

Below are just some of the things that the PPBF has been involved in supplying and fundraising for, to help both neonatal staff and parents with a baby receiving local hospital care:
If you would like to make a donation towards the PPBF’s local projects, you can do so here.